“My advice to anyone new to point-of-care ultrasound is that they should never be afraid to scan. The more often I use my Butterfly iQ Vet, the better I am at recognizing abnormalities.”
Today, ultrasound is more accessible than ever, and in an ideal world, should be considered an extension of the physical exam. But when I first purchased my Butterfly iQ Vet, I was cautious. I knew ultrasound could help my practice, but I hadn’t held a probe since veterinary school.
New technology can be intimidating, and you might not know where to begin. There are in-person courses, online classes, and video tutorials, but for many of us, the question is where and how to start.
This case is just one example of a patient I treated after I started using my Butterfly iQ Vet. Despite my limited background in performing point-of-care ultrasound (POCUS), I was quickly able to integrate POCUS into my practice, identify a problem, and treat it more effectively than I would have otherwise.
A five-month-old male kitten arrived with left rear lameness, a swollen thigh, and fever. The client came in for a second opinion after two weeks of kitten presenting worsening symptoms. At the patient’s first veterinary visit, radiography appeared normal, lab work was performed, and antibiotics were administered, but symptoms were not resolved. The leg had grown larger and the kitten was in greater pain, with difficulty walking. The previous veterinarian had provided a differential diagnosis of cancer.
Repeat radiography was not desired due to cost and radiation, so I used my Butterfly iQ Vet as an alternative. Under POCUS examination, an abscess on the thigh was apparent. Most feline abscesses are subcutaneous and can be identified by skin discoloration, but this cat’s skin was normal over the swollen site.
I compared the abscess to the normal contralateral limb to confirm these findings. The abscess was aspirated under ultrasound, but residual contents remained. The client returned the following day to lance the abscess under anesthesia. The abscess was re-imaged and at subsequent visits. Residual swelling was present, but no complex fluid collections were identified.
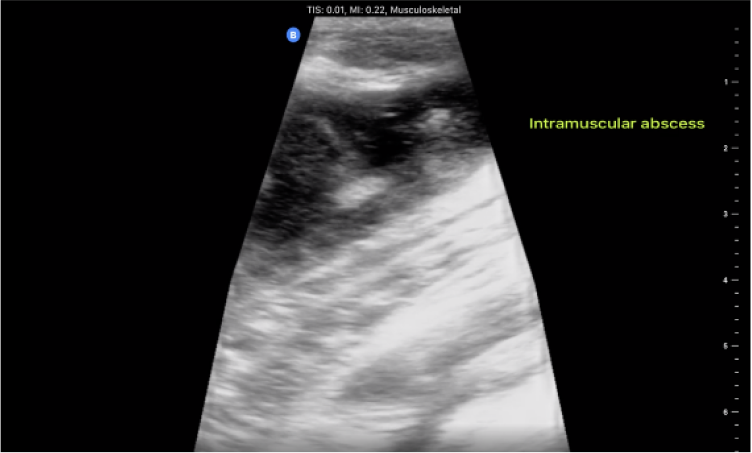

Point-of-care ultrasound was a cost-effective way to identify something unseen. I was able to use POCUS throughout care – to identify the source of the issue, to perform a procedure to address it immediately, and to monitor the patient’s improvement over time. This new skill can be applied to most of my patients’ assessments, not limited to bladder, A-FAST, and T-FAST evaluation.
My advice to anyone new to point-of-care ultrasound is that they should never be afraid to scan. The more often I use my Butterfly iQ Vet, the better I am at recognizing abnormalities. For this patient, that ability to recognize and confirm an abnormality saved time and money. I was able to immediately diagnose the issue, relieve the patient of discomfort, and develop a plan for care.
I’ve found the Butterfly iQ Vet to be invaluable to integrate POCUS into my practice. It has improved my patient care, helped me teach myself, and added additional revenue to my practice - learning how to do just 3 types of scans allows me to bring imaging as a tool to tens of patients every week that I otherwise wouldn’t. I wasn’t an expert before, and in just a few months I’ve gained skills that have directly benefited my patients and my practice.
Kramer M, Gerwing M, Hach V, Schimke E. Sonography of the musculoskeletal system in dogs and cats. Vet Radiol Ultrasound. 1997;38(2):139-149. doi:10.1111/j.1740-8261.1997.tb00829.x https://pubmed.ncbi.nlm.nih.gov/9238783/
Leonard CA, Tillson M. Feline lameness. Vet Clin North Am Small Anim Pract. 2001;31(1):143‐vii. doi:10.1016/s0195-5616(01)50042-x https://pubmed.ncbi.nlm.nih.gov/11787258/